One in seven patients discharged from Wollongong Hospital last year said they did not feel well enough to leave, according to the results of a new survey.
Subscribe now for unlimited access.
or signup to continue reading
And just over one in six patients were readmitted to the hospital, or had to go back to the emergency department, within one month because of complications related to the care they received.
The Bureau of Health Information's new report into patients' experiences in NSW hospitals reveals most rated their overall care highly in 2021, despite challenging conditions during the pandemic.
In Wollongong, 94 per cent rated their doctors as good or very good, while nurses got a 97 per cent approval rating.
Results were similar at Shellharbour Hospital, with doctors rated as good or very good in 95 per cent of cases, and nurses receiving 97 per cent approval.
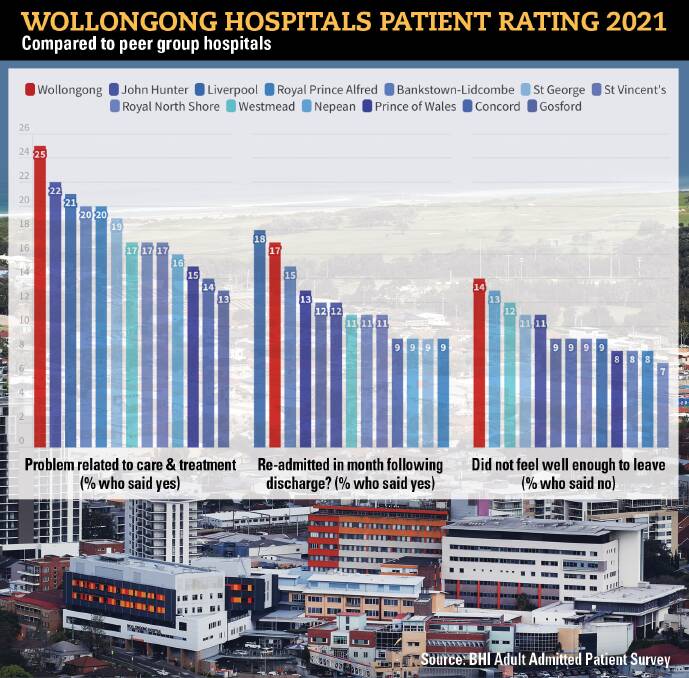
However 25 per cent of Wollongong Hospital patients said they experienced a problem related to their care and treatment during or very soon after their stay.
And for 83 per cent of these patients, the impact of the problem was very serious (37%) or fairly serious (44%).
Released on Wednesday, the results of the Adult Admitted Patient Survey 2021 reflect the experiences of 19,304 adults who received care in one of 87 NSW public hospitals.
In most categories, the standard of care for Wollongong and Shellharbour hospitals was around average compared to the state, with neither rating significantly higher, or lower than other hospitals in terms of overall care.
However, Wollongong had the second highest rate of readmissions due to complications (17%) in the state, behind only Liverpool Hospital where 18 per cent of patients said they needed to be readmitted or return to the ED within a month.
It also had the lowest number of patients (86 per cent) of any hospital in the state who said they felt well enough to leave by the time they were discharged, and was the state's worst performer (equal with Mona Vale rehabilitation hospital) when it came to the number of patients experiencing a problem with their care.
Wollongong hospital's challenges have continued this year, with data released in September showing the Illawarra's main hospital performed worst in the state compared to similar hospitals, when it came to median waiting times for patients needing to be admitted.
One in ten patients needing a bed waited more than 26 hours and 49 minutes to leave Wollongong ED, that data showed, and Wollongong also had the highest number of patients who left before being treated, compared to hospitals in its peer group.
Asked about the stand-out figures in the patient survey, Illawarra Shoalhaven Local Health District Chief Executive Margot Mains did not comment, but highlighted that the region's hospitals had "responded to the significant challenges presented by the Delta and Omicron waves of COVID-19" during the survey period.
She highlighted that the survey showed 93 per cent of patients surveyed across the district rated their overall care as either 'very good' (67 per cent) or 'good' (26 per cent), and that 89 per cent said they were 'always' treated with respect and dignity while in hospital.
"The results show the remarkable efforts of our healthcare professionals and we continue to thank them for their hard work and commitment to providing high-quality care to our patients," she said.
"Patient experience is the responsibility of all our staff and is embedded in everything we do. The District has an ongoing focus on improving the delivery of safe, high-quality and patient-centred care and has a range of initiatives in place to support these improvements, including a focus on engaging directly with consumers."
BHI Chief Executive Dr Diane Watson also noted that the pandemic had led to significant changes in how services were delivered, with additional measures introduced to ensure patient and staff safety.
"COVID-19 restrictions may have affected experiences of care, particularly in the second half of the year with the peak of the Delta outbreak and the beginning of the Omicron wave," said Dr Watson.
"However, most patients were positive about their experiences during their hospital stay, around their discharge and with virtual care appointments afterwards."
We've made it a whole lot easier for you to have your say. Our new comment platform requires only one log-in to access articles and to join the discussion on the Illawarra Mercury website. Find out how to register so you can enjoy civil, friendly and engaging discussions. Sign up for a subscription here.


